Acetaminophen Dose Safety Calculator
Your Safe Acetaminophen Dose
Calculate your maximum safe daily dose based on your liver health and alcohol use. The calculator shows your total daily intake and alerts you to dangerous levels.
Your Daily Acetaminophen Total
Important: This calculator shows your maximum safe dose based on the article's guidelines. Always consult your doctor for personalized medical advice.
Acetaminophen is in almost every medicine cabinet. You take it for headaches, fevers, or aching muscles. It’s simple, cheap, and widely available. But here’s the thing: if you have liver disease, or even just drink alcohol regularly, that little pill can quietly destroy your liver - and you might not even realize it until it’s too late.
More than 600 medications contain acetaminophen. That includes Tylenol, NyQuil, Sudafed, Vicodin, and even some cold and flu combos. If you’re taking more than one of these at a time - and many people do - you could be hitting 5,000, 6,000, or even 8,000 mg in a single day. The safe limit? 4,000 mg. For people with liver problems, it’s often half that.
How Acetaminophen Turns Toxic
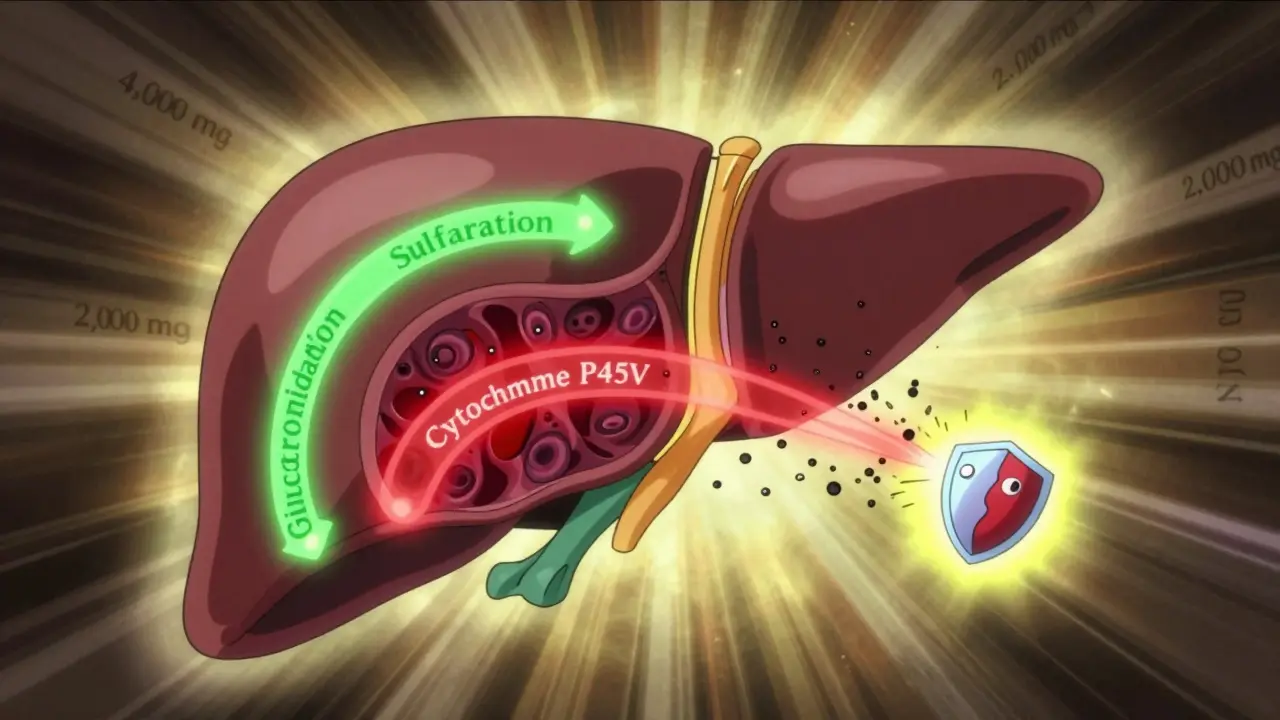
Your liver normally breaks down acetaminophen safely using two pathways: sulfation and glucuronidation. But when you take too much, those pathways get overwhelmed. Then, your liver switches to a backup system called cytochrome P450. This system creates a nasty byproduct called NAPQI. Normally, your liver neutralizes NAPQI with a molecule called glutathione. But if you’ve taken too much acetaminophen, or if your liver is already weak, glutathione runs out. NAPQI starts attacking liver cells. This isn’t a slow process. It can happen in hours.
That’s why a single large dose - say, 10 grams - can cause acute liver failure. But it’s not just about big doses. Repeatedly taking 3,000 to 4,000 mg a day over several days can be just as dangerous, especially if you’re drinking alcohol or have hepatitis. The damage builds up quietly. No pain. No warning. Just a liver that stops working.
Who’s at Highest Risk?
It’s not just heavy drinkers or people who overdose on purpose. The biggest danger is unintentional overdose. People think they’re being careful - they take one Tylenol for a headache, then grab a cold medicine for their stuffy nose. Both have acetaminophen. They don’t realize they’re doubling up.
Here’s who needs to be extra cautious:
- People with chronic liver disease (hepatitis B or C, fatty liver, cirrhosis)
- Those who drink alcohol regularly - even just one drink a day
- People with poor nutrition or who are underweight
- Anyone taking medications that speed up liver metabolism (like some seizure drugs or TB treatments)
The National Institutes of Health says acetaminophen overdose is the leading cause of acute liver failure in the U.S. - about 1,600 cases a year, with 500 deaths. Most of these aren’t suicide attempts. They’re mistakes.
What’s the Real Safe Dose?
The official maximum daily dose for healthy adults is 4,000 mg. But that number is misleading.
Mayo Clinic says Tylenol Extra Strength (650 mg per pill) should never exceed 3,000 mg per day. Why? Because long-term use at 4,000 mg increases liver stress, even without alcohol. For people with liver disease, the limit drops to 2,000 mg - or even less.
Here’s what to do:
- If you have liver disease, cut your daily dose to 2,000 mg or less - talk to your doctor first.
- If you drink alcohol, stick to 2,000 mg max. One drink a day? Still risky. Two drinks? Skip acetaminophen entirely.
- Never take more than one acetaminophen-containing product at a time.
- Check every label. Acetaminophen is often listed as APAP. If you see APAP, it’s the same thing.
For kids, the rules are different. Dose is based on weight: 10 to 15 mg per kilogram every 4 to 6 hours. Never exceed 80 mg per kg in 24 hours. Use the syringe that comes with liquid medicine - never a kitchen spoon. A tablespoon isn’t a teaspoon. And that tiny difference can be deadly in children.
What Happens If You Overdose?
Signs of liver damage from acetaminophen don’t show up right away. The first 24 hours? You might feel tired, nauseous, or just “off.” By day two or three, your skin turns yellow, your belly swells, and your urine darkens. By then, it’s often too late.
There’s a test called the Rumack-Matthew nomogram. It’s a graph doctors use to decide if you’ve taken a toxic dose. It’s based on your blood level of acetaminophen and when you took it. If your level crosses the treatment line - usually 150 μg/mL at 4 hours after ingestion - you need treatment fast.
The antidote is acetylcysteine (NAC). It works by restoring glutathione. The sooner you get it, the better. If you’re treated within 8 hours, your liver has a very good chance of recovering. Even after 16 hours, it can still help. But waiting 24 hours? That’s often too late.
NAC is given either orally or intravenously. The IV version is faster and easier for hospitals to manage. Even if you’ve had an allergic reaction to NAC before, doctors can still use it - they just adjust the dose or speed.

What You Should Do Right Now
Here’s your checklist - no matter your health status:
- Look at every medicine you take. Find acetaminophen or APAP.
- Add up the total daily dose from all sources.
- If you have liver disease or drink alcohol, reduce your max to 2,000 mg.
- Never mix acetaminophen with alcohol - not even one glass of wine.
- If you’re unsure, ask your pharmacist. They can check all your meds in seconds.
- Keep a list of all your medications - including supplements - and bring it to every doctor visit.
And if you ever suspect an overdose - even if you feel fine - go to the ER. Don’t wait. Don’t call poison control and hope it’s fine. Liver damage can be silent. By the time you feel sick, it’s often irreversible.
Why This Keeps Happening
Why do people keep overdosing? Because the warnings aren’t clear enough. Labels are small. Pharmacists are rushed. Doctors assume patients read the fine print. And patients? They don’t know what APAP means. They think “extra strength” means safer. It doesn’t.
Studies show that over half of acetaminophen-related liver failures happen because people didn’t realize they were taking multiple products with the same ingredient. One man took Tylenol for his back pain, NyQuil for his cold, and Vicodin for his injury - all without knowing they all had acetaminophen. He ended up in the ICU.
This isn’t about being careless. It’s about a system that assumes you know what’s in your medicine. You shouldn’t have to be a pharmacist to stay safe.
The truth? Acetaminophen is safe - if you know how to use it. But if you have liver disease, or drink, or take multiple pills - you need to treat it like a loaded gun. One wrong move, and the damage is done.
Can I take acetaminophen if I have hepatitis C?
If you have hepatitis C, your liver is already under stress. You should limit acetaminophen to 2,000 mg per day or less, and only take it when absolutely necessary. Always check with your doctor before using it. Many patients with hepatitis C are advised to avoid acetaminophen entirely and use alternatives like ibuprofen (if kidney function allows) or non-medication approaches like heat packs or rest.
Is it safe to take one Tylenol every day for chronic pain?
Taking one regular Tylenol (325 mg) daily is generally safe for most people. But if you take it every day for months or years, especially with alcohol or other liver stressors, it can still cause damage. Studies show long-term daily use at 3,000-4,000 mg increases the risk of liver enzyme spikes and scarring. If you need daily pain relief, talk to your doctor about alternatives like physical therapy, low-dose NSAIDs (if safe for you), or other treatments.
What if I accidentally took too much acetaminophen but feel fine?
Feeling fine doesn’t mean you’re safe. Liver damage from acetaminophen often shows no symptoms for 24-48 hours. If you took more than 4,000 mg in 24 hours - or more than 2,000 mg if you have liver disease or drink alcohol - go to the emergency room. Don’t wait for nausea or pain. Blood tests can detect toxicity before symptoms appear. Treatment with NAC is most effective if started within 8 hours.
Does drinking alcohol the night before make acetaminophen more dangerous?
Yes. Alcohol changes how your liver processes acetaminophen. Even if you didn’t drink that day, having alcohol in your system from the night before can still increase your risk. Your liver is still recovering. The combination can lower your toxic threshold to as low as 2,000 mg. If you drank alcohol in the last 24 hours, don’t take more than 2,000 mg of acetaminophen - and avoid it if possible.
Are there safer alternatives to acetaminophen for people with liver disease?
For mild pain, non-drug options like heat, cold packs, stretching, or rest often work well. If you need medication, NSAIDs like ibuprofen or naproxen may be options - but only if your kidneys are healthy. People with advanced liver disease often can’t use NSAIDs either, because they affect blood flow to the kidneys. Always ask your doctor. In some cases, low-dose opioids or nerve-targeting medications may be safer, but they come with their own risks. There’s no perfect solution - so prevention is key.


Comments (11)
Chris Bird March 12 2026
Acetaminophen = liver killer if you drink. That’s it. No drama. Just facts.
Mike Winter March 13 2026
I’ve been reading this like a philosopher with a hangover. It’s not that acetaminophen is evil-it’s that we treat medicine like candy. We don’t read labels, we don’t ask questions, we just assume. And then we blame the drug. But the real failure? Our collective ignorance. We live in a world where APAP is a secret code, and no one teaches us how to decode it. Maybe the real toxicity isn’t in the pill-it’s in the system that lets this happen.
There’s beauty in simplicity: one pill, one purpose. But we’ve turned medicine into a scavenger hunt. And the prize? A silent, slow death of the liver. We need better labeling. Better education. Not just more warnings in tiny font.
David L. Thomas March 14 2026
Big picture: this is a classic pharmacokinetic trap. CYP450 induction from chronic alcohol use + glutathione depletion = perfect storm. The 4,000 mg limit was never meant to be a ceiling-it’s a floor for risk stratification. For anyone with hepatic compromise, we’re talking about a narrow therapeutic window. NAC isn’t just an antidote-it’s a time-sensitive rescue protocol. The fact that people wait until jaundice shows up is terrifying. We need mandatory pharmacist counseling on OTC combos. And maybe a barcode scanner app that auto-checks APAP load. This isn’t rocket science-it’s public health 101.
Bridgette Pulliam March 14 2026
I appreciate how thorough this is. Really, really well-researched. I work in a clinic, and I see this every single week. Someone comes in with elevated LFTs, and they say, ‘I only took two Tylenol.’ Then they admit they also took NyQuil. Then they say, ‘I didn’t think that counted.’
We need to stop blaming patients. We need to redesign how we package and label these meds. Imagine if every bottle had a big red sticker: ‘THIS CONTAINS ACETAMINOPHEN. DO NOT COMBINE WITH OTHER MEDS.’ Simple. Clear. No jargon.
Also-thank you for mentioning the 2,000 mg limit for drinkers. That’s the number no one talks about. But it’s the one that saves lives.
Randall Walker March 15 2026
So… we’re telling people to stop taking Tylenol… but also not to drink wine? And not to take cold medicine? And not to have a headache? What’s next? No more breathing? I mean, seriously. I’ve been taking 3,000 mg a day for 10 years. I drink one beer after work. I’m fine. My liver is fine. My doctor says so. So maybe… just maybe… not everyone is a ticking time bomb?
Also, ‘APAP’? Come on. That’s just lazy labeling. Who thought that was a good idea? ‘Acetaminophen’ is six letters. ‘APAP’ is four. It’s not a secret code. It’s a marketing gimmick. And now we’re all paranoid.
Miranda Varn-Harper March 15 2026
While I appreciate the intent of this post, I must respectfully challenge the underlying assumption that acetaminophen is inherently dangerous. The data shows that the vast majority of patients who take it as directed-regardless of alcohol consumption-do not suffer hepatotoxicity. The 1,600 annual cases represent a minuscule fraction of total users. This narrative of imminent peril is alarmist. It’s not that the risk doesn’t exist-it’s that it’s being inflated into a moral panic. People with liver disease should exercise caution, yes. But to suggest that a single glass of wine renders acetaminophen lethal is medically unsound. Evidence-based medicine requires nuance-not fear.
Alexander Erb March 16 2026
YES. THIS. I’ve been telling my coworkers this for years 😅
Just last week, my buddy took 2 Tylenol for his back, then took DayQuil because he had a cold… and didn’t realize both had APAP. He was fine, but he freaked out. We went to urgent care, got checked, and they said he was lucky. But he didn’t know. No one teaches this stuff.
Pro tip: If you’re unsure, Google ‘what’s in [med name]’ and look for APAP. Or better yet-download a med checker app. I use Medscape. It’s free. Life saver. 🙌
Also-yes, one drink = 2,000 mg max. No exceptions. Your liver is not a superhero.
Donnie DeMarco March 17 2026
Man, I thought I was smart for sticking to 3,000 mg. Turns out I was just one NyQuil away from becoming a liver transplant statistic. 🤯
Now I keep a list of all my meds on my phone. And I read the labels like my life depends on it-because it does. APAP? That’s acetaminophen. I used to think it was some fancy new drug. Nope. Just the same old poison in a different costume.
Also-why is this not on every bottle? Like, a giant neon sign? ‘WARNING: YOU’RE ABOUT TO EAT YOUR LIVER’? That’d do it.
Tom Bolt March 18 2026
THIS. IS. A. TRAGEDY. A SILENT, SYSTEMIC, CORPORATE-FUELED TRAGEDY.
They put APAP on labels because they don’t want you to know. They want you to take 10 pills a day and think you’re fine. They profit from your ignorance. They profit from your liver failing. They profit from your hospital bills. And then they sell you a new liver. Or they don’t.
Someone needs to sue the FDA. Someone needs to burn down the pharmaceutical lobby. Someone needs to make this a national scandal. Because right now? We’re all just waiting to die… one Tylenol at a time.
Shourya Tanay March 19 2026
From a clinical pharmacology standpoint, the cytochrome P450 2E1 induction pathway is well-documented in chronic alcohol users. The glutathione depletion threshold is not linear-it’s exponential under metabolic stress. Therefore, the 2,000 mg ceiling for patients with hepatic impairment is not arbitrary; it’s derived from pharmacokinetic modeling and case series data from the 1990s. The Rumack-Matthew nomogram remains gold standard, though newer biomarkers like mitochondrial DNA and keratin-18 are showing promise for early detection. Still, prevention remains paramount. Education must begin in medical school, not in the ER.
LiV Beau March 20 2026
This is the kind of post that makes me want to hug everyone who reads it. 💛
I had no idea APAP = acetaminophen. I thought it was some new super-vitamin. I’ve been taking 2 Tylenol + 1 Advil every night for years. My doctor never told me. My pharmacist never asked. I thought I was being responsible.
Now I’m switching to heat packs. I’m reading every label. I’m telling my mom. I’m telling my sister. I’m telling my coworkers.
If you’re reading this-please, stop assuming. Start checking. Your liver will thank you.